| REVIEWED RECIPES |
| More popular recipes... |
| FEATURED |
| SPECIAL RECIPES |
| More featured recipes... |
U. S. Food and Drug Administration
FDA Consumer
January - February 1999
Keeping Cholesterol Under Control
by John Henkel
Cholesterol is the Jekyll and Hyde of the body.
Like the literary split personality, it has a good side because it is needed for certain important body functions. But for many Americans, cholesterol also has an evil side. When present in excessive amounts, it can injure blood vessels and cause heart attacks and stroke.
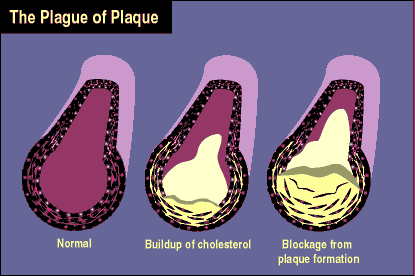
The body needs cholesterol for digesting dietary fats, making hormones, building cell walls, and other important processes. The bloodstream carries cholesterol in particles called lipoproteins that are like blood-borne cargo trucks delivering cholesterol to various body tissues to be used, stored or excreted. But too much of this circulating cholesterol can injure arteries, especially the coronary ones that supply the heart. This leads to accumulation of cholesterol-laden "plaque" in vessel linings, a condition called atherosclerosis.
When blood flow to the heart is impeded, the heart muscle becomes starved for oxygen, causing chest pain (angina). If a blood clot completely obstructs a coronary artery affected by atherosclerosis, a heart attack (myocardial infarction) or death can occur.
Heart disease is the number one killer of both men and women in this country. More than 90 million American adults, or about 50 percent, have elevated blood cholesterol levels, one of the key risk factors for heart disease, according to the National Heart, Lung, and Blood Institute's National Cholesterol Education Program.
While the institute estimates that heart disease killed nearly half a million in 1996, the most recent year for which figures are available, a study published in the New England Journal of Medicine in September 1998 says heart disease deaths have declined steadily over the last 30 years. Indeed, between 1990 and 1994, heart disease deaths decreased by 10.3 percent, the study says. From this and other studies, it appears that this is due largely to improvements in medical care after heart attack, a reduction in the number of repeat heart attacks, and better prevention of heart disease development.
A key factor in this drop is that the public, patients and doctors today are better informed about the risks associated with elevated cholesterol and the benefits of lifestyle changes and medical measures aimed at lowering blood cholesterol. "Public health initiatives such as the National Cholesterol Education Program have raised consumer awareness, promoted effective interventions, and have likely contributed to the reduction in heart disease deaths," says David Orloff, M.D., of the Food and Drug Administration's division of metabolic and endocrine drug products.
Another factor in the drop may be a relatively new class of drugs called statins. These have provided doctors with an arsenal of therapies to lower elevated blood cholesterol levels, often dramatically. To date, FDA has approved six statin drugs.
When Blood Cholesterol Becomes a Problem
Two types of lipoproteins and their quantity in the blood are main factors in heart disease risk:
- Low-density lipoprotein (LDL)--This "bad" cholesterol is the form in which cholesterol is carried into the blood and is the main cause of harmful fatty buildup in arteries. The higher the LDL cholesterol level in the blood, the greater the heart disease risk.
- High-density lipoprotein (HDL)--This "good" cholesterol carries blood cholesterol back to the liver, where it can be eliminated. HDL helps prevent a cholesterol buildup in blood vessels. Low HDL levels increase heart disease risk.
One of the primary ways LDL cholesterol levels can become too high in blood is through eating too much of two nutrients: saturated fat, which is found mostly in animal products, and cholesterol, found only in animal products. Saturated fat raises LDL levels more than anything else in the diet.
Several other factors also affect blood cholesterol levels:
- Heredity--High cholesterol often runs in families. Even though specific genetic causes have been identified in only a minority of cases, genes still play a role in influencing blood cholesterol levels.
- Weight--Excess weight tends to increase blood cholesterol levels. Losing weight may help lower levels.
- Exercise--Regular physical activity may not only lower LDL cholesterol, but it may increase levels of desirable HDL.
- Age and gender--Before menopause, women tend to have total cholesterol levels lower than men at the same age. Cholesterol levels naturally rise as men and women age. Menopause is often associated with increases in LDL cholesterol in women.
- Stress--Studies have not shown stress to be directly linked to cholesterol levels. But experts say that because people sometimes eat fatty foods to console themselves when under stress, this can cause higher blood cholesterol.
Though high total and LDL cholesterol levels, along with low HDL cholesterol, can increase heart disease risk, they are among several other risk factors. These include cigarette smoking, high blood pressure, diabetes, obesity, and physical inactivity. If any of these is present in addition to high blood cholesterol, the risk of heart disease is even greater.
The good news is that all these can be brought under control either by changes in lifestyle--such as diet, losing weight, or an exercise program--or quitting a tobacco habit. Drugs also may be necessary in some people. Sometimes one change can help bring several risk factors under control. For example, weight loss can reduce blood cholesterol levels, help control diabetes, and lower high blood pressure.
But some risk factors cannot be controlled. These include age (45 years or older for men and 55 years or older for women) and family history of early heart disease (father or brother stricken before age 55; mother or sister stricken before age 65).
What Is High Blood Cholesterol?
Cholesterol levels are determined through chemical analysis of a blood sample taken from a finger prick or from a vein in the arm. Home cholesterol kits, first approved in 1993, test only for total cholesterol levels but are as accurate as tests done in a doctor's office, says Steven Gutman, M.D., director of FDA's division of clinical laboratory devices. "These tests can give a consumer very valuable information when screening for high cholesterol," he says. "But they shouldn't be considered substitutes for a test conducted in a doctor's office." He adds that if test results are elevated, consumers should see a doctor right away for a more refined blood analysis. The National Cholesterol Education Program considers cholesterol testing in a doctor's office to be the preferred way because the patient can get advice immediately about the meaning of the results and what to do.
Besides determining total cholesterol levels, doctors often order a lipoprotein profile that shows the amounts of LDL, HDL, and another type of blood fat called triglycerides. This information gives doctors a better idea of heart disease risk and helps guide any treatment.
Cholesterol levels are measured in milligrams per deciliter (mg/dL). The National Cholesterol Education Program developed the following classifications for people over age 20 who do not have heart disease:
- Desirable blood cholesterol--Total blood cholesterol is less than 200 mg/dL; LDL is lower than 130 mg/dL.
- Borderline high cholesterol--Total level is between 200 and 239 mg/dL or LDL is 130 to 159 mg/dL.
- High blood cholesterol--Total level is greater than 240 mg/dL or LDL is 160 mg/dL or higher. For patients with heart disease, LDL above 100 mg/dL is too high. In addition, an HDL level less than 35 mg/dL is considered low and increases the risk of heart disease.
The main goal of cholesterol treatment is to lower LDL in people without heart disease. If the LDL level is in the "high" category and fewer than two other risk factors for heart disease are present, the goal is an LDL level lower than 160 mg/dL. If two or more risk factors are present, the goal is less than 130 mg/dL. If a patient already has heart disease, LDL levels should be 100 mg/dL or less. By reducing LDL, heart disease patients may prevent future heart attacks, prolong their lives, and slow down or even reverse cholesterol buildup in the arteries, according to the National Heart, Lung, and Blood Institute.
Treating High Blood Cholesterol
When a patient without heart disease is first diagnosed with elevated blood cholesterol, doctors often prescribe a program of diet, exercise, and weight loss to bring levels down. National Cholesterol Education Program guidelines suggest at least a six-month program of reduced dietary saturated fat and cholesterol, together with physical activity and weight control, as the primary treatment before resorting to drug therapy. Typically, doctors prescribe the Step I/Step II diet (see "Food for Thought") to lower dietary fat, especially saturated fat. Many patients respond well to this diet and end up sufficiently reducing blood cholesterol levels. Study data reinforce these benefits. For example, a 1998 Columbia University study examined 103 male and female patients of diverse ages and ethnic backgrounds and found that reducing dietary saturated fat directly affected blood cholesterol. For every 1 percent drop in saturated fat, the study showed a 1 percent lowering of LDL in patients.
But sometimes diet and exercise alone are not enough to reduce cholesterol to goal levels. Perhaps a patient is genetically predisposed to high blood cholesterol. In these cases, doctors often prescribe drugs. The National Cholesterol Education Program estimates that as many as 9 million Americans take some form of cholesterol-lowering drug therapy. The most prominent cholesterol drugs are in the statin family, an array of powerful treatments that includes Mevacor (lovastatin), Lescol (fluvastatin), Pravachol (pravastatin), Zocor (simvastatin), Baycol (cervastatin), and Lipitor (atorvastatin). Many doctors say statin drugs have revolutionized patient care.
"These drugs have had a fantastic impact on cholesterol treatment," says Redonda Miller, M.D., assistant professor of medicine at Johns Hopkins University School of Medicine. "They all lower cholesterol levels, but the side effects are minimal."
A study published in the medical journal Circulation in 1998 showed that statins dramatically lower the risk of dying from heart disease. Research found that for every 10 percentage points cholesterol was reduced, the risk of death from heart disease dropped by 15 percent.
So far, only three of the drugs--Mevacor, Zocor and Pravachol--have been studied in long-term, controlled trials. "Based on existing evidence, [statin drugs] all have similar safety profiles and are effective at lowering cholesterol in appropriately selected patients," says FDA's Orloff. "The difference between drugs lies mainly in their absolute capacity to lower cholesterol--that is, at the highest approved daily doses."
One landmark study completed in 1994, the Scandinavian Simvastatin Survival Study, or 4S, showed a 42 percent reduction in deaths from heart disease and a 30 percent drop in death from all causes over five years in patients with coronary heart disease whose high LDL levels were lowered with Zocor. The West of Scotland study, reported in 1995, revealed similar benefits from lowering LDL levels with Pravachol in patients without heart disease. And the Cholesterol and Recurrent Events (CARE) study, reported in 1996, showed that lowering LDL levels with Pravachol reduced heart attacks and deaths in patients with a previous heart attack but with cholesterol levels relatively average for the general population. This study showed that Pravachol treatment not only reduced death from heart disease but also death from all causes in a group of heart disease patients with average cholesterol levels.
A 1997 study, the Air Force/Texas Coronary Atherosclerosis Prevention Study, showed that Mevacor helped prevent a first heart attack or unstable angina in men and women with average cholesterol levels but with below-average HDL.
Statins work by interfering with the cholesterol-producing mechanisms of the liver and by increasing the capacity of the liver to remove cholesterol from circulating blood. Statins can lower LDL cholesterol by as much as 60 percent, depending on the drug and dosage.
Heart patient Norbert Hoffmann, 65, of Northfield, Minn., saw what he calls "a dramatic drop" in cholesterol levels after taking Zocor for three months. For example, his total cholesterol went from 270 to 145 mg/dL and LDL from 182 to 82 mg/dL.
But patients can respond differently to drugs. Some patients may have fewer side effects with one drug than another. "I had problems such as stomach cramps with Zocor," says Oklahoma patient Linden Gilbert, 50. His doctor ultimately switched him to Lipitor, which he credits with lowering his total cholesterol from 230 to 150 mg/dL.
Other Drug Treatments
These include:
- Nicotinic acid (niacin)-This lowers total and LDL cholesterol and raises HDL cholesterol. It also can lower triglycerides. Because the dose needed for treatment is about 100 times more than the Recommended Daily Allowance for niacin and thus can potentially be toxic, the drug must be taken under a doctor's care.
- Resins--Doctors have been prescribing Questran (cholestyramine) and Colestid (colestipol) for about 20 years. These "resins" bind bile acids in the intestine and prevent their recycling through the liver. Because the liver needs cholesterol to make bile, it increases its uptake of cholesterol from the blood.
- Fibric acid derivatives--Used mainly to lower triglycerides, Lopid (gemfibrozil) and Tricor (fenofibrate) can also increase HDL levels.
- Aspirin--Because studies have shown that aspirin can have a protective effect against heart attacks in patients with clogged blood vessels, doctors often prescribe the drug to patients with heart disease.
The decision of which drug to prescribe is one the doctor makes based on factors such as degree of cholesterol lowering desired, side effects, and cost. "If a patient has only a modest cholesterol elevation, I might prescribe Mevacor," says Johns Hopkins' Miller. "But if a more drastic reduction is needed, especially of LDL, I'll prescribe Lipitor."
The potential for drug interaction is a crucial concern, says FDA's Orloff. "Some statin drugs are known to interact adversely with other drugs, and that information may guide a decision about which statin to use." In June 1998, FDA announced the withdrawal of the drug Posicor (mibefradil), used to treat high blood pressure and stable angina, because it caused adverse reactions in patients taking various other drugs, including Mevacor and Zocor.
Though it is impossible to know yet just how many lives cholesterol-lowering therapies have saved, public health experts say awareness efforts such as the National Cholesterol Education Program are getting the word out to Americans about heart disease, its prevention and management. Reflecting on his own experience with elevated cholesterol, Hoffmann says, "Get informed [about cholesterol]. Read books, search the Internet, look at your risk factors, and, most of all, don't wait to do something about it if you have a [cholesterol] problem."
Food for Thought
One of the main ways blood cholesterol can reach undesirable levels is through a diet high in saturated fat and cholesterol. Fatty cholesterol deposits can collect in blood vessels, raising the risk of heart disease.
Drugs, exercise, and other therapies may be prescribed. But in many cases, cholesterol levels can be lowered by revising dietary habits and limiting the kinds of foods known to boost cholesterol, such as those high in saturated fat. This doesn't mean totally eliminating all your favorite foods, such as desserts, says the National Cholesterol Education Program (NCEP). It means taking a more prudent approach to the kinds and amounts of foods you eat.
When elevated cholesterol is first discovered in a person without heart disease, doctors often start patients on the Step I diet recommended by the American Heart Association and NCEP. On this program, patients should eat: 8 to 10 percent of the day's total calories from saturated fat, 30 percent or less of total calories from fat, less than 300 milligrams of dietary cholesterol a day, and just enough calories to achieve and maintain a healthy weight. A doctor or a registered dietitian can suggest a reasonable calorie level. Food labels also are very helpful in determining how much saturated fat, cholesterol, and calories are in various foods.
If the Step I diet doesn't result in desirable cholesterol levels, doctors may try the Step II diet, which changes the daily saturated fat limits to below 7 percent of daily calories and dietary cholesterol to below 200 milligrams. Step II also is the diet for people with heart disease.
In many patients, blood cholesterol levels should begin to drop a few weeks after starting on a cholesterol-lowering diet. Just how much of a drop depends on factors such as how high the cholesterol level is and how each person's body responds to changes made. With time, cholesterol levels may be reduced 10 to 50 milligrams per deciliter or more, a clinically significant amount.
| RECIPE PULSE |
| TRENDING NOW |